I’m so pleased to be hosting author Jocelyn Green this week. She e-mailed me a feasibility question and I managed to rope her into writing a few posts about the medical aspects of the Civil War!
I know…I’m a tricky girl.
Jocelyn has graciously agreed to give away a signed copy of her novel Wedded to War. Just leave a comment in the comments section that includes your e-mail address on any of her posts this week and you’ll be eligible to win– though must live in the USA. Drawing will be Saturday, September 1, 2012 at midnight. Winner announced here on Sunday, Sept 2, 2012!
Here is Part I and Part II.
It’s impossible to write a Civil War novel about medical care in the Union army without having at least some text devoted to amputations. Here’s some of the information that helped me as I wrote Wedded to War, and even now as I’m working on the next novel, Widow of Gettysburg.
Contrary to popular belief, the days of “biting the bullet” (or a leather strap) during an amputation were over by the time of the Civil War. Anesthesia was available in the form of chloroform and ether, even in field hospitals. However, if the soldier had been wounded more than 24 hours prior to amputation, the surgeon would not give anesthesia for fear the patient would not recover from it. And unfortunately, the Confederacy had a severe shortage of medicines, including these, to work with. So even though the medicine existed, there were plenty of cases where the patients had to go without it.
 |
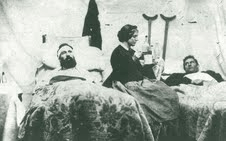
| Photo courtesy of Kevin Ling |
But in the cases where anesthesia was available, there were specific guidelines for how to administer it.
Chloroform
According to the Manual of Military Surgery Prepared for the Use of the Confederate States Army (published 1863):
· Chloroform should be given in the fresh air with the patient’s head on a pillow and the body remaining horizontal throughout inhalation.
· Clothing should be loosened about the neck, chest and abdomen so that breathing is not restricted.
· Only a light but nutritious meal should be given earlier, or the state of unconsciousness during the second stage of the anesthetic might bring on vomiting.
· Before giving the chloroform, first give brandy. (Union surgeons did not always follow this point. They used alcohol stimuli only on physically depressed patients because they felt it could slow down the induction of anesthesia in a healthy patient.)
The Confederate manual went on to instruct: “all special instruments of inhalation have been discarded, and a towel or napkin, folded into a cone, by having its corners turned down, is not almost universally employed for the purpose. The chloroform, about a drachm (one-eighth ounce) is poured into this cone, and is held over the patient’s mouth and nostrils which should previously have been anointed.” Holding the cone a half-inch from the patient’s face prevented facial blistering and allowed adequate air flow.
The first stage of anesthesia was one of excitement, producing “muttering, wild eyed, the cries, the exalted imagination” followed by “violent struggles, attempts to rise, and rigid contraction.” If the spasm extended to the larynx, there would be danger of breathing being obstructed. Surgeons were instructed to remove the cone temporarily if this were the case.
The second stage was that of unconsciousness, insensibility and relaxation of the voluntary muscles. Eyelids would no longer contract when touched. The pulse would slow and weaken, respiration became shallow and feeble.
Ether
Ether was slow-acting, had a foul smell patients objected to, and caused coughing. But it was frequently used in general hospitals where time was not as pressing, because, unlike chloroform, it did not cause vomiting, prostration or increased excitement.
It was also far less dangerous if the wrong dose was given. Throughout the Civil War, only four deaths were recorded from overdoses of ether, while chloroform’s rate was 5.4 deaths for every thousand that used it.
The Operation
The book, Civil War Medicine, by C. Keith Wilbur, M.D. has easy-to-understand explanations and diagrams of various types of amputations. Those interested in primary source material for the operations can thank SonoftheSouth.net for posting excerpts from The Practice of Surgery by Samuel Cooper, here: http://www.sonofthesouth.net/leefoundation/amputation.htmThe book, written in 1820, would have served as the how-to guide for surgeons in the beginning of the war. These online excerpts provide detailed instructions for amputation of legs, arms, fingers and toes, including photos of original Civil War instruments.
Carl Schurz, commander of the Union’s 11th Corps at Gettysburg, offers this account of amputations after the battle:
Most of the operating tables were placed in the open where the light was best some of them partially protected against the rain by tarpaulins or blankets stretched upon poles. There stood the surgeons their sleeves rolled up to the elbows, their bare arms as well as their linen aprons smeared with blood, their knives not seldom held between their teeth while they were helping a patient on or off the table, or had their hands otherwise occupied around them pools of blood and amputated arms or legs in heaps sometimes more than man high. Antiseptic methods were still unknown at that time. As a wounded man was lifted on the table often shrieking with pain as the attendants handled him the surgeon quickly examined the wound and resolved upon cutting off the injured limb. Some ether was administered and the body put in position in a moment. The surgeon snatched his knife from between his teeth where it had been while his hands were busy, wiped it rapidly once or twice across his blood stained apron and the cutting began. The operation accomplished the surgeon would look around with a deep sigh. and then—“Next!”
Recommended Sources:
For more in-depth study, in addition to the resources I listed on my last post, I recommend:
Cooper, Samuel. The Practice of Surgery. London: A and R Spottiswoode, 1820. Available at Google Books here: http://bit.ly/OvS97P.
Hamilton, Frank Hastings. A Practical Treatise on Military Surgery. New York: Balliere Brothers, 1861. Available at Google Books here: http://bit.ly/O72JCN
Teacher Tube video (5 min.) from the Museum of the Confederacy about amputations and artificial limbs. Not graphic at all. http://bit.ly/SZhlEF
I also did a post on ether and chloroform. You can find that here.
*********************************************************************************
A former military wife, Jocelyn Green authored, along with contributing writers, the award-winning Faith Deployed: Daily Encouragement for Military Wives and Faith Deployed . . . Again. Jocelyn also co-authored Stories of Faith and Courage from the Home Front, which inspired her first novel: Wedded to War. She loves Mexican food, Broadway musicals, Toblerone chocolate bars, the color red, and reading on her patio. Jocelyn lives with her husband Rob and two small children in Cedar Falls, Iowa.