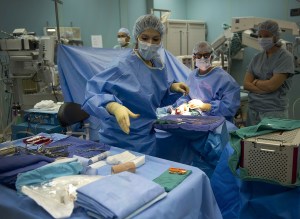
What happens when a surgeon takes out the wrong lung?
This writer’s question came from Lana and actually brings up several interesting points of discussion for her novel. First of all, the question stems from a family incident in 1954 which would really be considered historical as far as medicine is concerned.
Let’s dive into Lana’s question.
Lana asks:
I am a new writer and have some questions regarding a medical incident that occurred in my family in approximately 1954, but today the details are sketchy. Dr. Mabry (thanks Richard!) gave me your name.
The story: My uncle was told he had TB and must have his diseased lung removed. He had surgery, but the wrong lung was taken out.
Question #1: Would they have planned to remove the lung because of TB and would a doctor have actually taken out a whole lung or would it have been one lobe?
Question #2: Would the doctor have been able to see his mistake immediately after surgery? I’m not sure how the mistake was made or discovered.
Question #3: After removing the wrong lung (or lobe), how long would it have taken to reschedule another surgery?
Jordyn says:
One– I have to thank a physician coworker for her help on these– thanks, Liz!
Question #1: It depends on how diseased the lung was. Back then– there weren’t antibiotics to treat TB like there is now so this was considered treatment. However, since it didn’t cure the infection like antibiotics would– I’m not sure how beneficial it was for the patient. If on x-ray it looked like the whole lung was involved then they would have taken the whole thing out. If it looked like just part was involved– then perhaps just a lobe.
Question #2: The doctor would not have known about his mistake until the pathology report came back. The doctor I spoke to said on the outside– the lung might be very normal appearing (which perhaps played into the wrong lung being removed) but all removed biological things go to pathology to confirm a diagnosis. The wrong something being taken out or off is rare but does happen and lots of things play into these surgical errors. I’m going to provide some links below that talk about how these happen in some other situations.
Question #3: Reschedule surgery? Obviously– if they took out the whole lung he could not go back for another surgery to remove a whole other lung– because then he’d have nothing to do oxygen exchange and would therefore die. I guess they could remove part of the remaining lung but I’m not sure how much lung tissue you need to survive. This could be an area for you do some reading on. I couldn’t find a quick answer for you. It looks like the first successful lung transplant was in 1963 and it would have taken time for these procedures to become commonplace. If they did take him back– perhaps they’d wait for him to recover from the first surgery which might be a good 2-4 weeks I’m guessing.
Here are some links to this particular kind of surgery error:
http://www.nytimes.com/1995/09/17/us/doctor-who-cut-off-wrong-leg-is-defended-by-colleagues.html
http://www.cnn.com/2010/HEALTH/10/18/health.surgery.mixups.common/
http://www.lasvegassun.com/news/2011/jan/29/double-ouch-doctor-operates-wrong-knee/
Has anyone had this experience or known someone this has happened to? Did the hospital disclose why the error happened?
**************************************************************************
I’m Lana Kruse—last name pronounced Kruzey, rhymes with doozie! I’m one of the original baby boomers—you know, before we became a whole generation. It’s been fun to have been well-known, watched and written about since birth! I’m a wife, mother of two, grandmother of five (aka Mimi), and friend. I hope you will join me in that last category via my blog. I love people, words, laughter and eating out. Put all of these things together, and I’m in heaven!

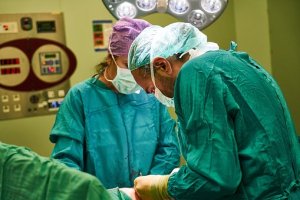 I have a few follow-up questions regarding the surgery. Is it possible for a thoracotomy to be done by two people? The hospital in my story is severely understaffed and only two doctors are available to perform the surgery. There are not enough nurses on staff either, and it’s the middle of the night. Is that feasible or should I tweak the story so more people are available to make sure the teen makes it out alive?
I have a few follow-up questions regarding the surgery. Is it possible for a thoracotomy to be done by two people? The hospital in my story is severely understaffed and only two doctors are available to perform the surgery. There are not enough nurses on staff either, and it’s the middle of the night. Is that feasible or should I tweak the story so more people are available to make sure the teen makes it out alive?