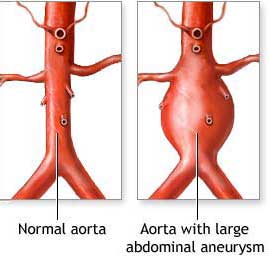
Dr. Edwards concludes his series on anuerysms today with a look at abdominal aneurysms.
The last blog in this series discussed problems with the upper (thoracic aorta) and how the condition known as a dissecting thoracic aorta can mimic heart attacks and be rapidly fatal if the wrong medication (a clot dissolving drug, for example) is given. This time we’re looking at the abdominal section of the aorta.
By far the most common emergency condition involving the abdominal aorta involves a ruptured aneurysm. An aneurysm means a ballooning. Abdominal aortic aneurysms, however, do not develop suddenly. They rupture suddenly, but the underlying problem—the development of a large bulging section—occurs slowly over years. We know that hypertension is a risk factor for this, but there are most likely hereditary factors as well. Typically the aneurysm begins in a person’s forties, fifties, sixties or later, and is often present, usually undetected, for ten years or more before reaching the dimensions (usually greater than 4 cm in diameter) where sudden rupture may occur.
Many, if not most, AAA’s remain asymptomatic and never rupture. If a physician discovers one on physical exam or finds one incidentally in the course of performing an ultrasound or a CT scan for an unrelated condition and the AAA is less than 4cm, the patient can be followed by repeat ultrasounds every six months or so. When and if the AAA reaches 4 cm, then consultation with a vascular surgeon is in order to consider a prophylactic graft procedure.
Unlike what happens with the thoracic aorta where a tear develops and blood channels inside the vessel wall, the AAA actually ruptures through the entire wall of the aorta and the patient can rapidly die from blood loss. Time is very much of the essence.
The classic presentation of a ruptured AAA will be a patient in their seventies or eighties with a long standing history of hypertension who has the acute onset of severe lower back or possibly flank area pain which may or may not extend around to the front of the abdomen. The pain is severe and a fair percentage of the time it is accompanied by a fainting episode and low blood pressure. In some ways the pain mimics that of a kidney stone, though I have personally seen two patients with a ruptured AAA that came in complaining of feeling constipated.
The diagnosis can be picked up by ultrasound or CT, but in a good number of cases, you can actually palpate a pulsatile mass in the abdomen. Emergency providers must keep a high index of suspicion for the presence of a ruptured AAA in any elderly patient with abdominal pain. If you don’t think about it, you can easily not consider it until the patient is crashing, and then it’s often too late. In general, though, it must be said that the mortality rate is very high even if the physician does everything right.
******************************************************************************

Frank Edwards was born and raised in Western New York. After serving as an Army helicopter pilot in Vietnam, he studied English and Chemistry at UNC Chapel Hill, then received an M.D. from the University of Rochester. Along the way he earned an MFA in Writing at Warren Wilson College. He continues to write, teach and practice emergency medicine. More information can be found at http://www.frankjedwards.com/.