Naomi Asks:
 My protagonist is a surgical resident at large hospital, and I want to write a scene where she is in the OR treating a piece of shrapnel entering the patient’s large intestine with no exit wound.
My protagonist is a surgical resident at large hospital, and I want to write a scene where she is in the OR treating a piece of shrapnel entering the patient’s large intestine with no exit wound.
It took quite a long time to get the patient any sort of medical attention and he has multiple myeloma. I’ve read from my research that myeloma can cause increase inflammation and compression of blood vessels causing coagulation and lessening internal bleeding.
A few questions:
I want to know the chance of my character surviving the surgery. I’m aware since there was no exit wound, and the piece of shrapnel didn’t hit any vital organs, that it would be high chance. However, since he received medical attention rather late (perhaps between half an hour and an hour) I want to know the chance of him actually surviving.
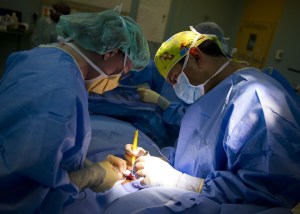 What would be the role of the surgical resident in this scenario? I don’t necessarily just want her to be cleaning up, but I want this to be as accurate as possible.
What would be the role of the surgical resident in this scenario? I don’t necessarily just want her to be cleaning up, but I want this to be as accurate as possible.
How long will it take to recover from this surgery?
Are they any complications that could happen during the surgery? If so, please list the major ones.
Jordyn Says:
For this question, I went to one of the best OR types I know . . . my friend Kim Zweygardt who works as a Certified Nurse Anesthetist (CRNA).
Kim Says:
First of all, let’s talk about length of time.
If the shrapnel missed all vital organs and major blood vessels, the length of time to treatment is minor. Are you talking from time of injury? If so, it takes some time for EMS to get to the scene, stabilize the patient, and get to the ER. It takes time in the ER for the nurses to start IVs, for the ER doctor to assess the patient, and get lab and radiology studies to diagnose. It takes time for the surgery to be scheduled and the OR crew to set up for the case.
In a large teaching hospital, is there an OR open or do they have to wait? If the patient isn’t bleeding out, it’s urgent but not life and death. It’s unlikely for the patient to be in the OR from time of injury in half an hour or even an hour. For instance, in a stat C-section with the patient and crew in house, it’s supposed to be decision to incision within thirty minutes and it’s sometimes difficult to hit that timeline. It takes time to transfer the patient and get the OR ready so I wouldn’t be concerned with that time affecting the outcome in this scenario.
Chances of surviving the operation? It’s kind of a misunderstanding that lots of people die in the OR! Your chances of surviving something is very good in the OR because everything and everybody is there to help you survive— all ways to stop bleeding, medications to resuscitate, etc.
The biggest risk is if the shrapnel was close to major blood vessels that could be nicked by the sharpness during removal. Most likely scenario is if it’s embedded in the bowel then they would just resect the bowel. In other words, remove the piece of bowel damaged along with the shrapnel. That’s normally done using a special stapler and then reconnected.
It’s possible depending on damage that they’d do a temporary colostomy. Let the bowel heal and go back later to reconnect it.
Biggest worry is infection. Normally when you resect the bowel you do a bowel prep so the colon is empty of stool. The shrapnel itself is dirty but having to resect an unprepped colon— risk of infection is very high and serious enough to cause death. But it’s not an immediate thing. They’d put him on antibiotics but within 24-48 hours he’d have symptoms if infected.
Role of the resident— depends on how advanced they are in their training. If early in residency, assisting. Holding retractors. If more advanced they could do most of the case. In all cases, if an attending surgeon is there, the resident will be left to close the surgical wound, write the orders for post op, and follow up on the patient in the ICU or PACU (Post Anesthesia Care Unit). What they wouldn’t do is clean things up! That is left to the nurses and techs.
His recovery time? If no infection then three to five days if healthy and their bowels are moving to where they can eat, drink, go to the bathroom, etc. With infection recovery time could be weeks or even a month or more.
Hope this helped and best of luck with your story!
******************************************************************************************
 Kimberly Zweygardt is a Christ follower, wife, mother, writer, blogger, dramatist, worship leader, Certified Registered Nurse Anesthetist, a fused glass artist and a taker of naps. Her writings have been featured in Rural Roads Magazine, The Rocking Chair Reader, and Chicken Soup for the Soul Healthy Living Series on Heart Disease. She is the author of Stories From the Well and Ashes to Beauty, The Real Cinderella Story and was featured in Stories of Remarkable Women of Faith. She lives in Northwest Kansas with her husband where their nest is empty but their lives are full. For more information: www.kimzweygardt.com.
Kimberly Zweygardt is a Christ follower, wife, mother, writer, blogger, dramatist, worship leader, Certified Registered Nurse Anesthetist, a fused glass artist and a taker of naps. Her writings have been featured in Rural Roads Magazine, The Rocking Chair Reader, and Chicken Soup for the Soul Healthy Living Series on Heart Disease. She is the author of Stories From the Well and Ashes to Beauty, The Real Cinderella Story and was featured in Stories of Remarkable Women of Faith. She lives in Northwest Kansas with her husband where their nest is empty but their lives are full. For more information: www.kimzweygardt.com.

 gospel truth of Jesus Christ. Her stories dive into the healthcare environment where Shannon holds over twenty years of experience as a Registered Diagnostic Medical Sonographer. Her extensive work experience includes Radiology, Obstetrics/Gynecology and Vascular Surgery.
gospel truth of Jesus Christ. Her stories dive into the healthcare environment where Shannon holds over twenty years of experience as a Registered Diagnostic Medical Sonographer. Her extensive work experience includes Radiology, Obstetrics/Gynecology and Vascular Surgery. My protagonist is a surgical resident at large hospital, and I want to write a scene where she is in the OR treating a piece of shrapnel entering the patient’s large intestine with no exit wound.
My protagonist is a surgical resident at large hospital, and I want to write a scene where she is in the OR treating a piece of shrapnel entering the patient’s large intestine with no exit wound. What would be the role of the surgical resident in this scenario? I don’t necessarily just want her to be cleaning up, but I want this to be as accurate as possible.
What would be the role of the surgical resident in this scenario? I don’t necessarily just want her to be cleaning up, but I want this to be as accurate as possible. Kimberly Zweygardt is a Christ follower, wife, mother, writer, blogger, dramatist, worship leader, Certified Registered Nurse Anesthetist, a fused glass artist and a taker of naps. Her writings have been featured in Rural Roads Magazine, The Rocking Chair Reader, and Chicken Soup for the Soul Healthy Living Series on Heart Disease. She is the author of Stories From the Well and Ashes to Beauty, The Real Cinderella Story and was featured in Stories of Remarkable Women of Faith. She lives in Northwest Kansas with her husband where their nest is empty but their lives are full. For more information:
Kimberly Zweygardt is a Christ follower, wife, mother, writer, blogger, dramatist, worship leader, Certified Registered Nurse Anesthetist, a fused glass artist and a taker of naps. Her writings have been featured in Rural Roads Magazine, The Rocking Chair Reader, and Chicken Soup for the Soul Healthy Living Series on Heart Disease. She is the author of Stories From the Well and Ashes to Beauty, The Real Cinderella Story and was featured in Stories of Remarkable Women of Faith. She lives in Northwest Kansas with her husband where their nest is empty but their lives are full. For more information:  It will make you hate hospitals and everything about them.
It will make you hate hospitals and everything about them. Episode 2 has so many issues it’s taking me two posts just to cover it.
Episode 2 has so many issues it’s taking me two posts just to cover it.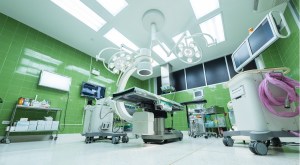 I have a question. I have had several surgeries, including foot surgery where a block was used. The list of medications on my bill were astounding! I understand the induction agent, narcotics and versed, but what is the anesthesia gas for? Just to keep the patient asleep? I love these posts!
I have a question. I have had several surgeries, including foot surgery where a block was used. The list of medications on my bill were astounding! I understand the induction agent, narcotics and versed, but what is the anesthesia gas for? Just to keep the patient asleep? I love these posts! Kimberly Zweygardt is a Christ follower, wife, mother, writer, blogger, dramatist, worship leader, Certified Registered Nurse Anesthetist, a fused glass artist and a taker of naps. Her writings have been featured in Rural Roads Magazine, The Rocking Chair Reader, and Chicken Soup for the Soul Healthy Living Series on Heart Disease. She is the author of Stories From the Well and Ashes to Beauty, The Real Cinderella Story and was featured in Stories of Remarkable Women of Faith. She lives in Northwest Kansas with her husband where their nest is empty but their lives are full. For more information:
Kimberly Zweygardt is a Christ follower, wife, mother, writer, blogger, dramatist, worship leader, Certified Registered Nurse Anesthetist, a fused glass artist and a taker of naps. Her writings have been featured in Rural Roads Magazine, The Rocking Chair Reader, and Chicken Soup for the Soul Healthy Living Series on Heart Disease. She is the author of Stories From the Well and Ashes to Beauty, The Real Cinderella Story and was featured in Stories of Remarkable Women of Faith. She lives in Northwest Kansas with her husband where their nest is empty but their lives are full. For more information:  Finally, the complication that movie nightmares are made of: recall under anesthesia.
Finally, the complication that movie nightmares are made of: recall under anesthesia. Anesthesia is sometimes defined as a controlled emergency. Here are some complications that would create great tension for our characters.
Anesthesia is sometimes defined as a controlled emergency. Here are some complications that would create great tension for our characters. We’ve all read about wrong patient or wrong operation or surgeons operating on the opposite leg, hip, etc. Safegaurds, like the time out, are designed to prevent this, but what if it increases plot tension?
We’ve all read about wrong patient or wrong operation or surgeons operating on the opposite leg, hip, etc. Safegaurds, like the time out, are designed to prevent this, but what if it increases plot tension?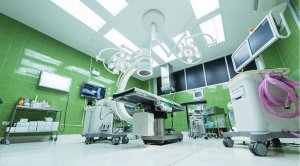 The OR is a cold, sterile, hard surface, brightly lit environment that is all about the task instead of comfort. Cabinets hold supplies, the operating room bed is called a table, Mayo stands hold instruments for immediate use during the operation and stainless steel wheeled tables hold extra instruments and supplies. IV poles, wheeled chairs/stools and the anesthesia machine and anesthesia cart complete the setting.
The OR is a cold, sterile, hard surface, brightly lit environment that is all about the task instead of comfort. Cabinets hold supplies, the operating room bed is called a table, Mayo stands hold instruments for immediate use during the operation and stainless steel wheeled tables hold extra instruments and supplies. IV poles, wheeled chairs/stools and the anesthesia machine and anesthesia cart complete the setting.