As I shared in my last post, I was working as a nurse during the COVID-19 pandemic– at the very dawn of it. Looking back, many I know are very blase about what it really was and what happened. It doesn’t help that each political side dug into their version, and it seems transparency and truth telling have succumbed to political power.

I cannot tell you how brave every front-line healthcare worker was to show up to work every day dealing with the unknown. From first responders (firefighters, police, and EMS), to CNA’s, to nurses, to respiratory therapists, and to doctors. Many health professionals assisted in any way they could– perhaps operating outside of their normal comfort zone just to save lives. Everyone who was working was putting their lives at risk. We didn’t know clearly how COVID-19 spread, what were the best therapies to treat, and what patients were more at risk. We were operating in darkness.
At the beginning of the pandemic, it looked very dire for those that went into the hospital. In those early days, if you ended up on a ventilator, you had a very high risk of mortality. Estimates vary wildly but let’s say a median good guess was around 75%. That’s not great.
My mother-in-law, who just turned 94 this year, visits us twice per year between her Minnesota and Arizona stays (yes, she’s a snowbird). In 2020, I told my husband I didn’t believe it was wise to have her come and stay with us as I didn’t want to be the one responsible for giving her an illness that no one knew who would live or die. She bypassed us and went to stay with her son and daughter-in-law that live in Cedar Rapids, Iowa.
I breathed a sigh of relief, thinking she was safe. None of them work in healthcare.
What happens? They all get COVID. My then 90 y/o mother-in-law, her son, my sister-in-law, and my niece. Age ranges from 20 to 90. Who gets sickest and needs to be hospitalized? My brother-in-law ended up needing to be on the ventilator. Knowing the early statistics as I did, I told my husband to brace himself. That this may not turn out very well. He thought I was being my normal, crazy, psychotic, healthcare worker that over-exaggerates everything (which, of course, I’m not. He just doesn’t have the inbred worry of every healthcare provider out there).
The good news is that my brother-in-law, after being intubated for three days, was extubated and is 90% recovered from the illness. To this day, he still has some lingering effects. My sister-in-law and niece got ill but didn’t require hospitalization. The least affected? My mother-in-law who got some slight sniffles.
A couple of years after, my husband was doing some reading on the pandemic and came to me and said, “I see why you were so worried about my brother. You were right– lots of people died in those early days who were put on the vent.”
It’s easy to look back in hindsight and think that what all of us who were heavily involved in the pandemic lived through turned out to be no big deal, but it was a VERY big deal.
Lots of death. We honestly didn’t know if we would be next. Think about this and please don’t ever tell a healthcare worker who lived through those early days that what they experienced what “no big deal”.
If you’re a healthcare worker, I’m curious as to what your experience was in those early days of COVID-19. I’d love for you to share your thoughts looking back. What do you want people to know?







 We’ve all read about wrong patient or wrong operation or surgeons operating on the opposite leg, hip, etc. Safegaurds, like the time out, are designed to prevent this, but what if it increases plot tension?
We’ve all read about wrong patient or wrong operation or surgeons operating on the opposite leg, hip, etc. Safegaurds, like the time out, are designed to prevent this, but what if it increases plot tension? Kimberly Zweygardt is a Christ follower, wife, mother, writer, blogger, dramatist, worship leader, Certified Registered Nurse Anesthetist, a fused glass artist and a taker of naps. Her writings have been featured in Rural Roads Magazine, The Rocking Chair Reader, and Chicken Soup for the Soul Healthy Living Series on Heart Disease. She is the author of Stories From the Well and Ashes to Beauty, The Real Cinderella Story and was featured in Stories of Remarkable Women of Faith. She lives in Northwest Kansas with her husband where their nest is empty but their lives are full. For more information:
Kimberly Zweygardt is a Christ follower, wife, mother, writer, blogger, dramatist, worship leader, Certified Registered Nurse Anesthetist, a fused glass artist and a taker of naps. Her writings have been featured in Rural Roads Magazine, The Rocking Chair Reader, and Chicken Soup for the Soul Healthy Living Series on Heart Disease. She is the author of Stories From the Well and Ashes to Beauty, The Real Cinderella Story and was featured in Stories of Remarkable Women of Faith. She lives in Northwest Kansas with her husband where their nest is empty but their lives are full. For more information: 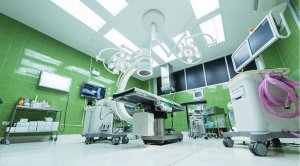 The OR is a cold, sterile, hard surface, brightly lit environment that is all about the task instead of comfort. Cabinets hold supplies, the operating room bed is called a table, Mayo stands hold instruments for immediate use during the operation and stainless steel wheeled tables hold extra instruments and supplies. IV poles, wheeled chairs/stools and the anesthesia machine and anesthesia cart complete the setting.
The OR is a cold, sterile, hard surface, brightly lit environment that is all about the task instead of comfort. Cabinets hold supplies, the operating room bed is called a table, Mayo stands hold instruments for immediate use during the operation and stainless steel wheeled tables hold extra instruments and supplies. IV poles, wheeled chairs/stools and the anesthesia machine and anesthesia cart complete the setting. If you have a profession besides writing, doesn’t it bug you when someone doesn’t get it right? It may be something small, but you wonder, “Why didn’t they do some research?” With the Internet, it is easier than ever to find information, but if it is a hidden profession like my own, there might not be much info for you to glean. Today I want to share with you, The Face Behind the Mask or The Life and Times of a Certified Registered Nurse Anesthetist (CRNA). The operating room is my world, so let’s begin there.
If you have a profession besides writing, doesn’t it bug you when someone doesn’t get it right? It may be something small, but you wonder, “Why didn’t they do some research?” With the Internet, it is easier than ever to find information, but if it is a hidden profession like my own, there might not be much info for you to glean. Today I want to share with you, The Face Behind the Mask or The Life and Times of a Certified Registered Nurse Anesthetist (CRNA). The operating room is my world, so let’s begin there. This year marks the Sesquicentennial (150-year anniversary) of the beginning of the Civil War. If you’ve never studied it much, I recommend you use these four commemorative years as an incentive to expand your knowledge of it.
This year marks the Sesquicentennial (150-year anniversary) of the beginning of the Civil War. If you’ve never studied it much, I recommend you use these four commemorative years as an incentive to expand your knowledge of it. Erin Rainwater is a Pennsylvania native whose trip to Gettysburg when she was twelve enhanced her already deep interest in the Civil War. She attended Duquesne University in Pittsburgh, and entered the Army Nurse Corps upon graduation. Serving during the Vietnam War era, she cared for the bodies and spirits of soldiers and veterans, including repatriated POWs and MIAs. Now living in Colorado, she is a member of a Disaster Medical Assistance Team, and has been deployed to disaster areas around the country.
Erin Rainwater is a Pennsylvania native whose trip to Gettysburg when she was twelve enhanced her already deep interest in the Civil War. She attended Duquesne University in Pittsburgh, and entered the Army Nurse Corps upon graduation. Serving during the Vietnam War era, she cared for the bodies and spirits of soldiers and veterans, including repatriated POWs and MIAs. Now living in Colorado, she is a member of a Disaster Medical Assistance Team, and has been deployed to disaster areas around the country.  That being said, I was mildly disappointed in a medical scene portrayed in Season 1, Episode 11. If you haven’t seen it, I don’t think I’ll be spoiling much unless you don’t the the fate of Toby post his Christmas collapse. If that statement is true then you should stop reading here.
That being said, I was mildly disappointed in a medical scene portrayed in Season 1, Episode 11. If you haven’t seen it, I don’t think I’ll be spoiling much unless you don’t the the fate of Toby post his Christmas collapse. If that statement is true then you should stop reading here. US Army Nursing in World War II—Part 3
US Army Nursing in World War II—Part 3 Sarah Sundin is the author of the Wings of Glory series from Revell:
Sarah Sundin is the author of the Wings of Glory series from Revell: